
A | B | C | D | E | F | G | H | CH | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | 0 | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9
| Fatigue | |
|---|---|
| Other names | Exhaustion, weariness, tiredness, lethargy, listlessness |
 | |
| Specialty | Primary care |
| Treatment | Avoid known stressors and unhealthy habits (drug use, excessive alcohol consumption, smoking), healthy diet, exercise regularly, medication, hydration, and vitamins |
Fatigue describes a state of tiredness (which is not sleepiness), exhaustion[1] or loss of energy.[2][3]
In general usage, fatigue often follows prolonged physical or mental activity. When fatigue occurs independently of physical or mental exertion, or does not resolve after rest or sleep, it may have other causes, such as a medical condition.[4]
Fatigue (in the medical sense) is associated with a wide variety of conditions including autoimmune disease, organ failure, chronic pain conditions, mood disorders, heart disease, infectious diseases, and post-infectious-disease states.[5] However fatigue is complex and in up to a third of primary care cases no medical or psychiatric diagnosis is found.[6][7][8]
Fatigue (in the general usage sense of normal tiredness) can include both physical and mental fatigue. Physical fatigue results from muscle fatigue brought about by intense physical activity.[9][10][11] Mental fatigue results from prolonged periods of cognitive activity which impairs cognitive ability. Mental fatigue can manifest as sleepiness, lethargy, or directed attention fatigue,[12] and can also impair physical performance.[13]
Definition
Fatigue in a medical context is used to cover experiences of low energy that are not caused by normal life.[2][3]
A 2021 review proposed a definition for fatigue as a starting point for discussion: "A multi-dimensional phenomenon in which the biophysiological, cognitive, motivational and emotional state of the body is affected resulting in significant impairment of the individual's ability to function in their normal capacity".[14]
Another definition is that fatigue is "a significant subjective sensation of weariness, increasing sense of effort, mismatch between effort expended and actual performance, or exhaustion independent from medications, chronic pain, physical deconditioning, anaemia, respiratory dysfunction, depression, and sleep disorders".[15]
Terminology
The use of the term "fatigue" in medical contexts may carry inaccurate connotations from the more general usage of the same word. More accurate terminology may also be needed for variants within the umbrella term of fatigue.[16]
Comparison with other terms
Tiredness
Tiredness which is a normal result of work, mental stress, anxiety, overstimulation and understimulation, jet lag, active recreation, boredom, or lack of sleep is not considered medical fatigue. This is the tiredness described in MeSH Descriptor Data.[17]
Sleepiness
Sleepiness refers to a tendency to fall asleep, whereas fatigue refers to an overwhelming sense of tiredness, lack of energy, and a feeling of exhaustion. Sleepiness and fatigue often coexist as a consequence of sleep deprivation.[18] However sleepiness and fatigue may not correlate.[19] Fatigue is generally considered a longer-term condition than sleepiness (somnolence).[20]
Features
Common features
Distinguishing features of medical fatigue include
- unpredictability,
- not linking fatigue to an obvious cause, such as a physical exertion,
- variability in severity,
- fatigue being relatively profound/overwhelming, and having extensive impact on daily living,
- lack of improvement with rest,
- where an underlying disease is present, the quantum of fatigue often does not correlate with the severity of the underlying disease.[14][21][22][23]
Characteristics by cause
Differentiating characteristics of fatigue that may help identify the possible cause of fatigue include
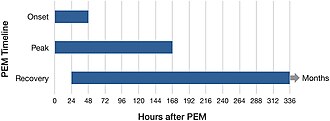
- Post-exertional malaise; a common feature of ME/CFS,[24] and experienced by a significant proportion of people with Long Covid,[25] but not a feature of other fatigues.
- Increased by heat or cold; MS fatigue is in many cases effected in this way.[26][27]
- Remission; MS fatigue may reduce during periods of other MS symptom remission.[28][29] ME/CFS may also have lower periods of activity.[30]
- Cognitive declines; sleep deprivation causes cognitive and neurobehavioral effects including unstable attention and slowing of response times.[31] ME/CFS and MS may cause brain fog over longer timescales.
- Intermittency; Fatigues often vary in how and when they occur. Some fatigues (RA, cancer fatigue[32]) seem to often be continual (24/7) whilst others (MS, Sjögren's, lupus, brain injury[33]) are often intermittent.[34] A 2010 study found that Sjögren's patients reported fatigue after rising, an improvement in mid-morning, and worsening later in the day, whereas lupus (SLE) patients reported lower fatigue after rising followed by increasing fatigue through the day.[35] ME/CFS symptoms can be continual, or can fluctuate during the day, from day to day, and over longer periods.[30]
- The pace of onset may be a related differentiating factor; MS fatigue can have abrupt onset.[36]
Some people may have multiple causes of fatigue.
Classification
By type
Uni- or multi-dimensional
Fatigue can be seen as a uni-dimensional phenomenon that influences different aspects of human life.[37][38] It can be multi-faceted and broadly defined, making understanding the causes of its manifestations especially difficult in conditions with diverse pathology including autoimmune diseases.[39]
A 2021 review considered that different "types/subsets" of fatigue may exist and that patients normally present with more than one such "type/subset". These different "types/subsets" of fatigue may be different dimensions of the same symptom, and the relative manifestations of each may depend on the relative contribution of different mechanisms. Inflammation may be the root causal mechanism in many cases.[14]
Physical
Physical fatigue, or muscle fatigue, is the temporary physical inability of muscles to perform optimally. The onset of muscle fatigue during physical activity is gradual, and depends upon an individual's level of physical fitness – other factors include sleep deprivation and overall health.[40] Physical fatigue can be caused by a lack of energy in the muscle, by a decrease of the efficiency of the neuromuscular junction or by a reduction of the drive originating from the central nervous system, and can be reversed by rest.[41] The central component of fatigue is triggered by an increase of the level of serotonin in the central nervous system.[42] During motor activity, serotonin released in synapses that contact motor neurons promotes muscle contraction.[43] During high level of motor activity, the amount of serotonin released increases and a spillover occurs. Serotonin binds to extrasynaptic receptors located on the axonal initial segment of motor neurons with the result that nerve impulse initiation and thereby muscle contraction are inhibited.[44]
Muscle strength testing can be used to determine the presence of a neuromuscular disease, but cannot determine its cause. Additional testing, such as electromyography, can provide diagnostic information, but information gained from muscle strength testing alone is not enough to diagnose most neuromuscular disorders.[45]
Mental
Mental fatigue is a temporary inability to maintain optimal cognitive performance. The onset of mental fatigue during any cognitive activity is gradual, and depends upon an individual's cognitive ability, and also upon other factors, such as sleep deprivation and overall health.
Mental fatigue has also been shown to decrease physical performance.[12] It can manifest as somnolence, lethargy, directed attention fatigue, or disengagement. Research also suggests that mental fatigue is closely linked to the concept of ego depletion, though the validity of the concept is disputed. For example, one pre-registered study of 686 participants found that after exerting mental effort, people are likely to disengage and become less interested in exerting further effort.[46]
Decreased attention can also be described as a more or less decreased level of consciousness.[47] In any case, this can be dangerous when performing tasks that require constant concentration, such as operating large vehicles. For instance, a person who is sufficiently somnolent may experience microsleep. However, objective cognitive testing can be used to differentiate the neurocognitive deficits of brain disease from those attributable to tiredness.[48][49][50]
The perception of mental fatigue is believed to be modulated by the brain's reticular activating system (RAS).[51][52][53][54][55]
Fatigue impacts a driver's reaction time, awareness of hazards around them and their attention. Drowsy drivers are three times more likely to be involved in a car crash, and being awake over 20 hours is the equivalent of driving with a blood-alcohol concentration level of 0.08%.[56]
Neurological fatigue
People with multiple sclerosis experience a form of overwhelming tiredness that can occur at any time of the day, for any duration, and that does not necessarily recur in a recognizable pattern for any given patient, referred to as "neurological fatigue", and often as "multiple sclerosis fatigue" or "lassitude".[57][58][59]
People with autoimmune diseases including inflammatory rheumatic diseases such as rheumatoid arthritis, psoriatic arthritis and primary Sjögren's syndrome, experience similar fatigue.[14][39] Attempts have been made to isolate causes of central nervous system fatigue.
By timescale
Acute
Acute fatigue is that which is temporary and self-limited. Acute fatigue is most often caused by an infection such as the common cold and can be cognized as one part of the sickness behavior response occurring when the immune system fights an infection.[60]
Other common causes of acute fatigue include depression and chemical causes, such as dehydration, poisoning, low blood sugar, or mineral or vitamin deficiencies.
Prolonged
Prolonged fatigue is a self-reported, persistent (constant) fatigue lasting at least one month.[61][62]
Chronic
Chronic fatigue is a self-reported fatigue lasting at least 6 consecutive months. Chronic fatigue may be either persistent or relapsing.[63] Chronic fatigue is a symptom of many chronic illnesses and of idiopathic chronic fatigue.[medical citation needed]
By effect
Fatigue can have significant negative impacts on quality of life.[64][65] Profound and debilitating fatigue is the most common complaint reported among individuals with autoimmune disease, such as systemic lupus erythematosus, multiple sclerosis, type 1 diabetes, celiac disease, Myalgic Encephalomyelitis/chronic fatigue syndrome, and rheumatoid arthritis.[14]
Fatigue has been described by sufferers as 'incomprehensible' due to its unpredictable occurrence, lack of relationship to physical effort and different character as compared to tiredness.[66]
Fatigue that dissociates by quantum with disease activity represents a large health economic burden and unmet need to patients and to society.[14]
Formal classification
The World Health Organization's ICD-11 classification[67] includes a category MG22 Fatigue (typically fatigue following exertion but sometimes may occur in the absence of such exertion as a symptom of health conditions), and many other categories where fatigue is mentioned as a secondary result of other factors.[68] It does not include any fatigue-based psychiatric illness (unless it is accompanied by related psychiatric symptoms).[69][70]
DSM-5 lists 'fatigue or loss of energy nearly every day' as one factor in diagnosing depression.[71]
Measurement
Fatigue is currently measured by many different self-measurement surveys.[72] One example is the Fatigue Severity Scale.[73][74][75] There is no consensus on best practice,[76] and the existing surveys do not capture the intermittent nature of some forms of fatigue.
Nintendo announced plans for a device to possibly quantitatively measure fatigue in 2014,[77] but the project was stopped in 2016.[78]
Causes
Drug use
Caffeine and alcohol can cause fatigue.[79] A 2023 Korean study found that alcohol consumption was the variable with the most significant impact on overall fatigue.[80] A 2020 Norway study found that 69% of substance use disorder patients had severe fatigue symptoms.[81]
Unknown
In up to a third of fatigue primary care cases no medical or psychiatric diagnosis is found.[6][7][8] Tiredness is a common medically unexplained symptom.[7]
Sleep disturbanceedit
Fatigue can often be traced to poor sleep habits.[82] Sleep deprivation and disruption is associated with subsequent fatigue.[83][84] Sleep disturbances due to disease may impact fatigue.[85][86]
Medicationsedit
Fatigue may be a side effect of certain medications (e.g., lithium salts, ciprofloxacin); beta blockers, which can induce exercise intolerance, medicines used to treat allergies or coughs[82]) and many cancer treatments, particularly chemotherapy and radiotherapy.
Psychological stress and conditionsedit
Adverse life events have been associated with fatigue.[14]
Association with diseases and illnessesedit
Fatigue is often associated with diseases and conditions. Some major categories of conditions that often list fatigue as a symptom include physical diseases, substance use illness, mental illnesses, and other diseases and conditions.
Physical diseasesedit
- autoimmune diseases,[39] such as celiac disease, lupus, multiple sclerosis,[87] myasthenia gravis, NMOSD, Sjögren's syndrome,[35] rheumatoid arthritis,[88][89] spondyloarthropathy and UCTD;[90] this population's primary concern is fatigue;[39][91]
- blood disorders, such as anemia and hemochromatosis;[medical citation needed]
- brain injury;[92][93]
- cancer, in which case it is called cancer fatigue;[94]
- Covid-19 and long Covid;[95]
- developmental disorders such as autism spectrum disorder;[96]
- endocrine diseases or metabolic disorders: diabetes mellitus, hypothyroidism and Addison's disease;[97]
- fibromyalgia;[medical citation needed]
- heart failure and heart attack;[98]
- HIV;[medical citation needed]
- inborn errors of metabolism such as fructose malabsorption;[99][100]
- infectious diseases such as infectious mononucleosis or tuberculosis;[97]
- irritable bowel syndrome;[medical citation needed]
- kidney diseases, e.g., acute renal failure, chronic renal failure;[97]
- leukemia or lymphoma;[medical citation needed]
- liver failure or liver diseases, e.g., hepatitis;[97][22]
- Lyme disease;[medical citation needed]
- myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS);[101]
- neurological disorders such as narcolepsy, Parkinson's disease, postural orthostatic tachycardia syndrome (POTS) and post-concussion syndrome;[medical citation needed]
- physical trauma and other pain-causing conditions, such as arthritis;[medical citation needed]
- sleep deprivation or sleep disorders, e.g. sleep apnea;[97]
- stroke;[medical citation needed]
- thyroid disease such as hypothyroidism;[medical citation needed]
Substance use illnessesedit
- substance use disorders including alcohol use disorder;[102]
Mental illnessesedit
- anxiety disorders, such as generalized anxiety disorder;[103]
- depression;[104][14]
- eating disorders, which can produce fatigue due to inadequate nutrition;[medical citation needed]
- Gulf War syndrome;[medical citation needed]
Otheredit
- idiopathic chronic fatigue, a term used to describe chronic fatigue which does not have symptoms of ME/CFS.[105][106] However ICF does not have a dedicated diagnostic code in the World Health Organization's ICD-11 classification.[107]
Primary vs. secondaryedit
In some areas it has been proposed that fatigue be separated into primary fatigue, caused directly by a disease process, and ordinary or secondary fatigue, caused by a range of causes including exertion and also secondary impacts on a person of having a disease (such as disrupted sleep).[108][109][110][111][112][113] The ICD-11 MG22 definition of fatigue[114] captures both types of fatigue; it includes fatigue that "occurs in the absence of... exertion... as a symptom of health conditions."[medical citation needed]
Obesityedit
Obesity correlates with higher fatigue levels and incidence.[115][116][117]
Somatic symptom disorderedit
In somatic symptom disorder[118] the patient is overfocused on a physical symptom, such as fatigue, that may or may not be explained by a medical condition.[119][120][121]
Scientifically unsupported causesedit
The concept of adrenal fatigue is often raised in media but no scientific basis has been found for it.[122][123][124]
Mechanismsedit
The mechanisms that cause fatigue are not well understood.[39] Several mechanisms may be in operation within a patient,[125] with the relative contribution of each mechanism differing over time.[14]
Some mechanisms proposed as active in fatigue are inflammation, heat shock proteins and reduced brain connectivity.
Inflammationedit
Inflammation distorts neural chemistry, brain function and functional connectivity across a broad range of brain networks,[126] and has been linked to many types of fatigue.[39][127] Findings implicate neuroinflammation in the etiology of fatigue in autoimmune and related disorders.[14][39] Low-grade inflammation may cause an imbalance between energy availability and expenditure.[128]
Cytokines are small protein molecules that modulate immune responses and inflammation (as well as other functions) and may have causal roles in fatigue.[129][130] However a 2019 review was inconclusive as to whether cytokines play any definitive role in ME/CFS.[131]
The inflammation model may have difficulty in explaining the "unpredictability" and "variability" (i.e. appearing intermittently during the day, and not on all days) of the fatigue associated with inflammatory rheumatic diseases and autoimmune diseases (such as multiple sclerosis).[14]
Heat shock proteinsedit
A small 2016 study found that primary Sjögren's syndrome patients with high fatigue, when compared with those with low fatigue, had significantly higher plasma concentrations of HSP90α, and a tendency to higher concentrations of HSP72.[132] A small 2020 study of Crohn's disease patients found that higher fatigue visual analogue scale (fVAS) scores correlated with hgher HSP90α levels.[133] A related small 2012 trial investigating if application of an IL-1 receptor antagonist (anakinra) would reduce fatigue in primary Sjögren's syndrome patients was inconclusive.[134][135][136]
Reduced brain connectivityedit
Fatigue has been correlated with reductions in structural and functional connectivity in the brain.[137] This has included in post-stroke,[138] MS,[139] NMOSD and MOG,[15] and ME/CFS.[140] This was also found for fatigue after brain injury,[141] including a significant linear correlation between self-reported fatigue and brain functional connectivity.[142]
Areas of the brain for which there is evidence of relation to fatigue are the thalamus and middle frontal cortex,[142] fronto-parietal and cingulo-opercular,[141] and default mode network, salience network, and thalamocortical loop areas.[137][143]
Damage to brain white matteredit
Studies have found MS fatigue correlates with damage to NAWM (normal appearing white matter) (which will not show on normal MRI but will show on DTI (diffusion tensor imaging)).[144][145][146][147][148][149] The correlation becomes unreliable due to ageing in patients aged over 65.[150] Similar functional connectivity alterations related to fatigue may occur in NMOSD and MOG antibody disease.[151]
Prevalenceedit
2023 guidance stated fatigue prevalence is between 4.3% and 21.9%. Prevalence is higher in women than men.[6][152]
A 2021 German study found that fatigue was the main or secondary reason for 10–20% of all consultations with a primary care physician.[153]
A large study based on the 2004 Health and Retirement Study (HRS), a biennial longitudinal survey of US adults aged 51 and above, with mean age 65, found that 33% of women and 29% of men self-reported fatigue.[154]
Diagnosisedit
This section needs more reliable medical references for verification or relies too heavily on primary sources. (April 2024) |  |
2023 guidance[6] stated the following:
- in the primary care setting, a medical or psychiatric diagnosis is found in at least two-thirds of patients;
- the most common diagnoses are viral illness, upper respiratory infection, iron-deficiency anaemia, acute bronchitis, adverse effects of a medical agent in the proper dose, and depression or other mental disorder, such as panic disorder, and somatisation disorder;
- the origin of fatigue may be central, brain-derived, or peripheral, usually of a neuromuscular origin—it may be attributed to physical illness, psychological (e.g., psychiatric disorder), social (e.g., family problems), and physiological factors (e.g., old age), occupational illness (e.g., workplace stress);
- when unexplained, clinically evaluated chronic fatigue can be separated into ME/CFS and idiopathic chronic fatigue.[6]
A 2016 German review found that
- about 20% of people complaining of tiredness to a GP (general practitioner) suffered from a depressive disorder.
- anaemia, malignancies and other serious somatic diseases were only very rarely found in fatigued primary care patients, with prevalence rates hardly differing from non-fatigued patients.
- if fatigue occurred in primary care patients as an isolated symptom without additional abnormalities in the medical history and in the clinical examination, then extensive diagnostic testing rarely helped detect serious diseases. Such testing might also lead to false-positive tests.[155]
A 2014 Australian review recommended that a period of watchful waiting may be appropriate if there are no major warning signs.[156]
A 2009 study found that about 50% of people who had fatigue received a diagnosis that could explain the fatigue after a year with the condition. In those people who had a possible diagnosis, musculoskeletal (19.4%) and psychological problems (16.5%) were the most common. Definitive physical conditions were only found in 8.2% of cases.[157]
Treatment and Managementedit
Management may include review of existing medications, and other factors and methods explained below.
Review of existing medicationsedit
Medications may be evaluated for side effects that contribute to fatigue[158] [82][159][better source needed] and the interactions of medications are complex.[non-primary source needed][160]
Medications to treat fatigueedit
The UK NICE recommends consideration of amantadine, modafinil and SSRIs for MS fatigue.[161] Psychostimulants such as methylphenidate, amphetamines, and modafinil have been used in the treatment of fatigue related to depression,[162][163][164][165] and medical illness such as chronic fatigue syndrome[166][167] and cancer.[163][168][169][170][171][172][173] They have also been used to counteract fatigue in sleep loss[174] and in aviation.[175]
Mental health toolsedit
CBT has been found useful for fatigue.[176]
Improved sleepedit
Improving sleep can reduce fatigue.[177][178]
Zdroj:https://en.wikipedia.org?pojem=ExhaustedText je dostupný za podmienok Creative Commons Attribution/Share-Alike License 3.0 Unported; prípadne za ďalších podmienok. Podrobnejšie informácie nájdete na stránke Podmienky použitia.
Antropológia
Aplikované vedy
Bibliometria
Dejiny vedy
Encyklopédie
Filozofia vedy
Forenzné vedy
Humanitné vedy
Knižničná veda
Kryogenika
Kryptológia
Kulturológia
Literárna veda
Medzidisciplinárne oblasti
Metódy kvantitatívnej analýzy
Metavedy
Metodika
Text je dostupný za podmienok Creative
Commons Attribution/Share-Alike License 3.0 Unported; prípadne za ďalších
podmienok.
Podrobnejšie informácie nájdete na stránke Podmienky
použitia.
www.astronomia.sk | www.biologia.sk | www.botanika.sk | www.dejiny.sk | www.economy.sk | www.elektrotechnika.sk | www.estetika.sk | www.farmakologia.sk | www.filozofia.sk | Fyzika | www.futurologia.sk | www.genetika.sk | www.chemia.sk | www.lingvistika.sk | www.politologia.sk | www.psychologia.sk | www.sexuologia.sk | www.sociologia.sk | www.veda.sk I www.zoologia.sk
